Medicaid coverage for therapy is a crucial lifeline for individuals with limited financial means seeking essential medical services, including mental health care. The complex landscape of Medicaid coverage and its impact on therapy, particularly for children like B.T., who require consistent care, highlights the need for a holistic approach to well-being. Legislation such as Pennsylvania's Mental Health Parity and Addiction Equity Act aims to ensure that mental health services receive the same importance as physical health services.
As the demand for mental health care increases, it becomes vital for parents to understand Medicaid's coverage specifics and navigate the system effectively. Furthermore, finding therapists who accept Medicaid can be daunting, but online directories and telehealth services have made the search more accessible. Understanding evidence-based therapy and the qualifications of therapists is essential to secure appropriate care.
Lastly, selecting a Medicaid therapist requires careful consideration of licensure, qualifications, experience, and establishing a strong therapeutic relationship. As the demand for mental health services continues to grow, informed decisions about mental health care providers become increasingly important.
Medicaid, as a cornerstone of the American healthcare system, provides a lifeline to those with limited financial means, ensuring they get essential medical services, including mental health care. This becomes especially important in the context of treatment, where ongoing and easily available care can make a significant difference. The story of B.T., a nine-year-old from Florida with autism, exemplifies the importance of steadfast support. Despite her need for regular speech therapy, bureaucratic shifts led to a reduction in her treatment frequency, highlighting the challenges within the system.
The role of Medicaid is not just to provide coverage but also to ensure that the quality of care is not compromised by fiscal constraints. As the National Committee for Quality Assurance and Medicare have acknowledged the wider social determinants of well-being, the significance of a comprehensive approach to overall well-being, including stable housing and nutrition, has been underscored. This comprehension is critical as we contemplate Medicaid's approach to mental services.
For parents navigating this landscape, it is paramount to understand the coverage specifics of Medicaid when it comes to therapy. With Medicaid and CHIP being the primary source of coverage for nearly 90 million Americans, including many children, the implications of are significant. Pennsylvania's Parity Act and comparable laws across states strive to guarantee that [psychological well-being care](https://rori.care/post/10-effective-strategies-for-parents-to-boost-their-childs-social-skills) is given equal significance as physical medical care.
As the world becomes more conscious of the crucial importance of psychological well-being, particularly in the aftermath of the COVID-19 outbreak, there is an increasing demand for enhanced availability to psychological services. This has translated into legislative action, with policymakers now more attuned to the fiscal and social imperatives of psychological well-being coverage.
Comprehending the complex network of parity in psychological well-being, the varieties of insurance coverage accessible, and the entitlements of those insured is a crucial initial stride in obtaining suitable care. The complexity of navigating these systems underscores the need for clear information and support for those seeking therapy under Medicaid.
With statistics indicating that a significant portion of working-age adults in poverty remain uninsured, and with the ACA's goal to broaden access to healthcare, it's clear that there's a pressing need to address both financial and non-financial barriers to care. Access to psychological well-being assistance, as emphasized in the 'Enhancing Psychological Well-being Care in America: The Access Report,' is a critical domain where state policymakers can have an impact, guaranteeing that individuals like B.T. receive the consistent and quality care they deserve.
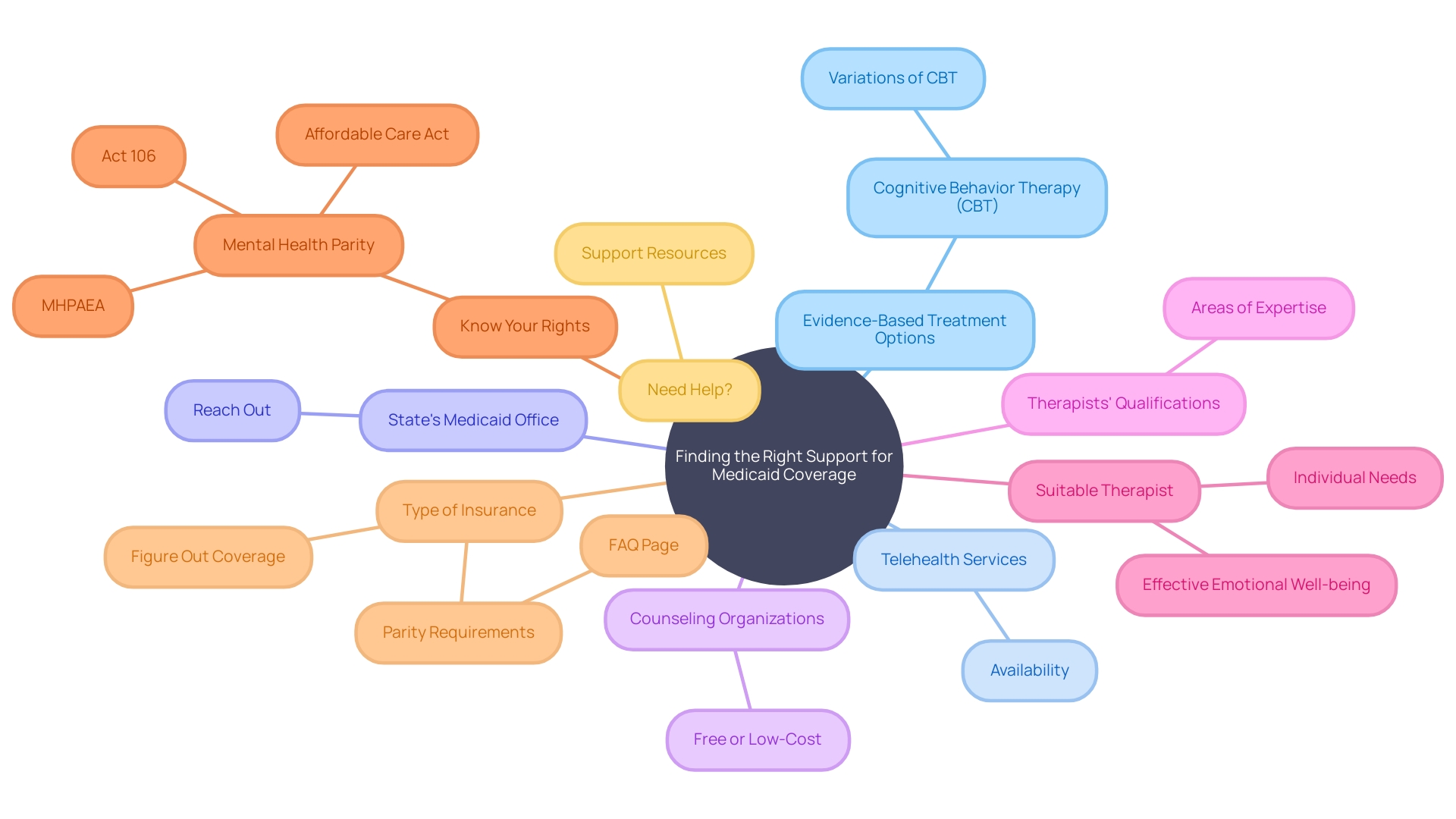
Finding the right support for Medicaid coverage can be overwhelming, particularly when searching for providers who accept Medicaid. To improve your search efficiency, it's crucial to be knowledgeable about evidence-based treatment, which indicates treatments scientifically proven to enhance mental health. Cognitive Behavior Therapy (CBT), for example, is a widely recognized form of evidence-based treatment, along with its variations tailored to specific conditions. Additionally, the recent expansion in telehealth services has broadened the selection of therapists available, allowing for more accessible care. While reaching out to your state's Medicaid office is a conventional method, investigating can also offer assistance for common conditions like anxiety and depression. It's crucial to be aware of therapists' qualifications and areas of expertise, as therapy costs can vary widely based on these factors. As you begin this journey, keep in mind the significance of finding a therapist who suits your needs to ensure the most effective path to emotional well-being.
Navigating the intricate terrain of psychological well-being services can be challenging, particularly when seeking therapists who accept Medicaid. Fortunately, online directories like Psychology Today and GoodTherapy have eased this process by offering search filters tailored to Medicaid recipients. These platforms not only simplify the search but also provide comprehensive profiles showcasing each therapist's expertise, credentials, and how to reach them.
With the changing dynamics of healthcare, especially the concerning increase in emotional well-being problems observed by BetterHelp and comparable platforms, the requirement for available therapy is crucial. The expansion of Medicare to include marriage and family therapists and counselors is a pivotal move, opening doors for many in need. This shift could not be more timely, with the pandemic highlighting the importance of psychological well-being and propelling telemedicine into the spotlight.
As you sift through potential therapists, understanding evidence-based therapy is paramount. Treatments like and its derivatives, including Mindfulness-Based Cognitive Therapy and Trauma-Focused CBT, are backed by research confirming their effectiveness in improving mental health. The growing utilization of telehealth has expanded the group of therapists accessible, providing more choices than ever before.
Cost can be a barrier to accessing treatment, with average session prices ranging from $60 to $200. Nevertheless, there are no-cost or affordable options accessible for typical concerns such as anxiety and depression, and numerous insurance policies provide coverage for mental health care, as required by the Affordable Care Act. The parity laws ensure that co-pays for therapy are not significantly higher than those for other medical procedures.
The introduction of telehealth services across state lines is further easing access, although regulations can vary by state. Despite these progressions, more than 50% of adults with psychological disorders did not receive treatment in 2020, frequently because of a scarcity of professionals in the field. This fact emphasizes the significance of comprehending the varied credentials of providers in the field of psychology to make well-informed choices.
Lastly, a recent 'secret shopper' study suggests that although telemedicine options vary among clinics, availability does not appear to be affected by perceived race, ethnicity, or psychological well-being. This implies a promising direction towards inclusiveness in telemedicine services, which have become a fundamental aspect in the psychological well-being landscape after the global health crisis.
Selecting a Medicaid therapist necessitates careful consideration to ensure you receive the highest quality care. It's crucial to confirm that the therapist has the required licensure and possesses the qualifications necessary to address your specific emotional well-being challenges. Experience plays a significant role as well; a therapist with a background in treating similar concerns can offer more tailored care. For example, if you are dealing with trauma or psychosis, it's beneficial to choose someone with specialized training in these areas.
Establishing a connection with your therapist is also vital, as a strong therapeutic relationship contributes to the effectiveness of your treatment. Considering the logistics, such as whether you prefer in-person sessions at a clinic or , can influence your comfort level and commitment to the process. The rise of telehealth options has expanded the pool of available therapists, making it easier to find a good match even if you have specific needs or preferences.
Furthermore, comprehending the categories of evidence-based therapies, such as Cognitive Behavior Therapy (CBT), Dialectical Behavior Therapy (DBT), or their variations, can assist you in selecting a therapist whose method is scientifically proven to enhance psychological well-being. As the demand for mental health services grows, evidenced by the expansion of New York State's mental health workforce and services, it's increasingly important to make informed decisions about your mental health care provider.

In conclusion, Medicaid coverage for therapy is crucial for individuals with limited financial means seeking mental health care. Legislation like Pennsylvania's Mental Health Parity and Addiction Equity Act aims to ensure that mental health services receive the same importance as physical health services. To navigate the system effectively, it's important for parents to understand Medicaid's coverage specifics.
Finding therapists who accept Medicaid can be daunting, but online directories and telehealth services have made the search more accessible. It's essential to be informed about evidence-based therapy, like Cognitive Behavior Therapy (CBT), and therapist qualifications for appropriate care.
Selecting a Medicaid therapist requires careful consideration of licensure, qualifications, experience, and a strong therapeutic relationship. The rise of telehealth options has expanded the pool of available therapists, making it easier to find a good match.
Informed decisions about mental health care providers are increasingly important as the demand for mental health services grows. By understanding evidence-based therapies and qualifications, parents can make the best choices for their children's mental health care. Remember, with the right knowledge and support, you can navigate the Medicaid system effectively and secure the quality care you deserve.
Find a Medicaid therapist easily with our online directory and telehealth services.
What is Medicaid's role in therapy coverage?
Medicaid provides essential medical services, including mental health care, to individuals with limited financial means. It aims to ensure that quality care is accessible despite fiscal constraints.
Why is understanding Medicaid coverage important for parents?
With nearly 90 million Americans covered by Medicaid and CHIP, knowing the specifics of coverage can help parents navigate treatment options for their children, ensuring they receive necessary therapy services.
What are some challenges faced by individuals seeking therapy through Medicaid?
Individuals may encounter bureaucratic shifts that affect treatment frequency and access to providers who accept Medicaid. Understanding coverage limitations is essential for effective navigation.
How has the demand for mental health services changed post-COVID-19?
There has been an increased awareness and demand for mental health services, prompting policymakers to focus on enhancing access to psychological well-being coverage.
What is the significance of insurance parity laws?
Insurance parity laws, like Pennsylvania's Parity Act, ensure that mental health care is treated equally to physical health care, promoting better access to necessary services.
How can individuals find therapists that accept Medicaid?
Individuals can use online directories like Psychology Today and GoodTherapy, reach out to their state's Medicaid office, or look into free or low-cost counseling organizations.
What types of therapy are recommended under Medicaid?
Evidence-based treatments, such as Cognitive Behavior Therapy (CBT) and its variations, are recommended as they are scientifically proven to enhance mental health.
What factors should be considered when choosing a Medicaid therapist?
Key considerations include the therapist's qualifications, experience with specific issues, the therapeutic relationship, and whether you prefer in-person or telehealth sessions.
How do telehealth services affect access to therapy?
The expansion of telehealth services has broadened the selection of therapists and improved accessibility, especially for those living in underserved areas.
What are the typical costs associated with therapy, and how does Medicaid help?
Therapy costs can range from $60 to $200 per session. Medicaid often covers mental health care as required by the Affordable Care Act, and parity laws ensure that co-pays for therapy are not significantly higher than those for other medical services.
What are the barriers to accessing mental health care?
Despite progress, many adults with psychological disorders remain untreated due to a lack of professionals, financial constraints, or insufficient awareness of available services.
How can individuals ensure they make informed choices about their mental health care?
Understanding the qualifications of providers, the types of therapies available, and the specifics of Medicaid coverage can empower individuals to make informed decisions about their mental health care.