The distinction between Asperger's Syndrome and Autism Spectrum Disorder (ASD) is rooted in the nuances of neurodevelopmental profiles. Historically, the term 'Asperger's Syndrome' traces back to the work of Hans Asperger, an Austrian pediatrician who observed children with certain social and communicative idiosyncrasies in the 1940s. However, recent scrutiny of Asperger's association with the Nazi regime's 'Kinder-Euthanasie' program has led to ethical concerns about eponymous naming in the medical community.
This article explores the historical context, current classification, key differences in symptoms and language development, social interaction and communication challenges, cognitive and behavioral patterns, language skills and pragmatic communication, intelligence and cognitive abilities, behavioral characteristics and repetitive behaviors, the importance of early diagnosis and individualized interventions, and treatment approaches for Asperger's and Autism. By understanding these aspects, parents and healthcare professionals can gain valuable insights into these conditions and empower themselves with expert advice to support individuals with ASD.
The difference between a specific type of [Autism Spectrum Disorder (ASD)](https://rori.care/services) and Autism Spectrum Disorder (ASD) is based on the intricacies of neurodevelopmental profiles. In the past, the term 'Asperger's Syndrome' can be attributed to the research conducted by Hans, an Austrian pediatrician who, during the 1940s, studied children with specific social and communicative peculiarities. However, recent scrutiny of Asperger's association with the Nazi regime's 'Kinder-Euthanasie' program has led to ethical concerns about eponymous naming in the medical community. In light of these revelations, there has been a shift towards non-eponymous terms to describe these conditions, reflecting a broader understanding that neurodiversity is an intrinsic part of personal identity rather than a disease. Autism, now recognized as a spectrum, presents in diverse forms, and there is no singular way to experience it. This modern perspective acknowledges that every autistic individual's experience is unique, and the spectrum is not defined by a linear severity scale but rather by the each person possesses.
The comprehension and categorization of the syndrome have undergone notable changes, especially with the release of the DSM-5 in 2013. Previously recognized as a distinct disorder, Asperger's Syndrome is now included within the broader diagnosis of Autism Spectrum Disorder (ASD). This integration reflects an effort to create a more inclusive framework for autism, acknowledging the diverse spectrum of symptoms and behaviors associated with the condition.
The evolution of this classification echoes a broader conversation in the medical community about the importance of precise and ethically considerate terminology. Based on an editorial stance from Pediatric Research, the medical field is moving away from eponymous names, especially when the historical background of the namesake is unclear or problematic. Moreover, this shift aligns with a deeper understanding of ASD as encompassing a range of possible features, which may not always be observable but are critical for diagnosis and support.
As ASD is conceptualized in ICD-11, it is characterized as a condition with a multitude of potential but not obligatory characteristics, challenging the clinical utility of previous definitions. The spectrum nature of ASD implies that it impacts people to different extents, influencing behavior, social skills, and communication. With estimates indicating that as many as 1 in 36 people may be on the spectrum, a unified diagnostic approach like the one in aids in offering resources and support customized to the specific requirements of each person.
These discussions and decisions in the medical community reflect a commitment to improving the lives of those with ASD and their families, ensuring that everyone, from friends and teachers to co-workers and strangers, can better understand and support individuals with autism throughout their lives.
Differentiating between a specific type of autism and Autism Spectrum Disorder (ASD) requires comprehending the subtleties in symptom intensity and language progress. A condition that falls under the broader ASD umbrella, typically presents with subtler symptoms. Individuals with Asperger's often maintain strong language abilities and exhibit normal intellectual development. However, ASD encompasses a range of challenges, with some people facing notable language delays and intellectual disabilities. These distinctions are crucial in accurately identifying and supporting the unique requirements of each person affected by these .

Comprehending the intricacies of social interaction and interaction in Asperger's Syndrome (AS) and Autism Spectrum Disorder (ASD) is essential, as these are fundamental difficulties for people within the spectrum. While both AS and ASD feature difficulties in these areas, the manifestation and intensity can vary. People with AS often find navigating social nuances like non-verbal cues and sustaining reciprocal relationships perplexing. They might misinterpret body language or the subtleties of conversation, leading to social misunderstandings.
In contrast, those with ASD may encounter more severe obstacles when attempting to initiate or maintain social exchanges. This could range from a lack of understanding of social constructs to a complete disinterest in participating in social activities. Based on research, people with autism are more prone to mental health issues and encounter larger obstacles in healthcare interaction, emphasizing the significance of customized patient engagement and care centered around the person.
A study emphasizes the barriers in exchanging information that individuals with autism encounter, indicating that acknowledging and utilizing their strengths in conveying messages can enhance interactions. For instance, some might excel in offering comfort or making requests, while others struggle with expressing personal feelings or engaging in small talk. Selecting the appropriate strategies for conveying messages, such as employing visuals or structured inquiries, can greatly enhance the exchange of information and emotional expression.
Moreover, recent discoveries indicate the crucial importance of comprehending the distinct interaction requirements of autistic adults to enhance their participation in care. Misalignments between perceptions and realities in healthcare settings can be addressed by focusing on the , ensuring their voices are central to their care.
Surprisingly, exposure to television and other media at a young age may impact the sensory processing of babies and toddlers, potentially leading to atypical sensory behaviors similar to those observed in ASD, such as disengagement or the need for intense stimulation. This highlights the complexity of sensory and language elements in ASD.
The societal misinterpretation of autistic communication patterns often leads to challenges in forming connections. However, by valuing the varied ways in which people on the autism spectrum process information and communicate, a more inclusive and empathetic environment can be cultivated, which is beneficial to the well-being of those on the spectrum.
Cognitive and behavioral patterns exhibit unique characteristics between people with Asperger's Syndrome and those with Autism Spectrum Disorder (ASD). People with Asperger's Syndrome tend to have intense interests in specific subjects and often pursue these passions with great dedication. For instance, they may become experts in areas like mathematics or have an exceptional talent for music. Additionally, they usually prefer routines and have a strong need for predictability in their daily lives.
Conversely, ASD encompasses a wider spectrum of cognitive abilities and behavioral patterns, making it a more heterogeneous condition. High functioning autism, a subset of ASD, generally refers to people who have a higher intellectual capacity and face fewer challenges in language and communication. However, these people may still face significant challenges in social situations, cope with sensory sensitivities, and display repetitive behaviors. The is a tool used during well-child visits to screen for autism. Even though the M-CHAT-R/F exhibits high specificity, its sensitivity is notably lower, indicating the necessity for more precise and universally accessible screening methods to improve early identification and intervention of autism, which can lead to more favorable outcomes.

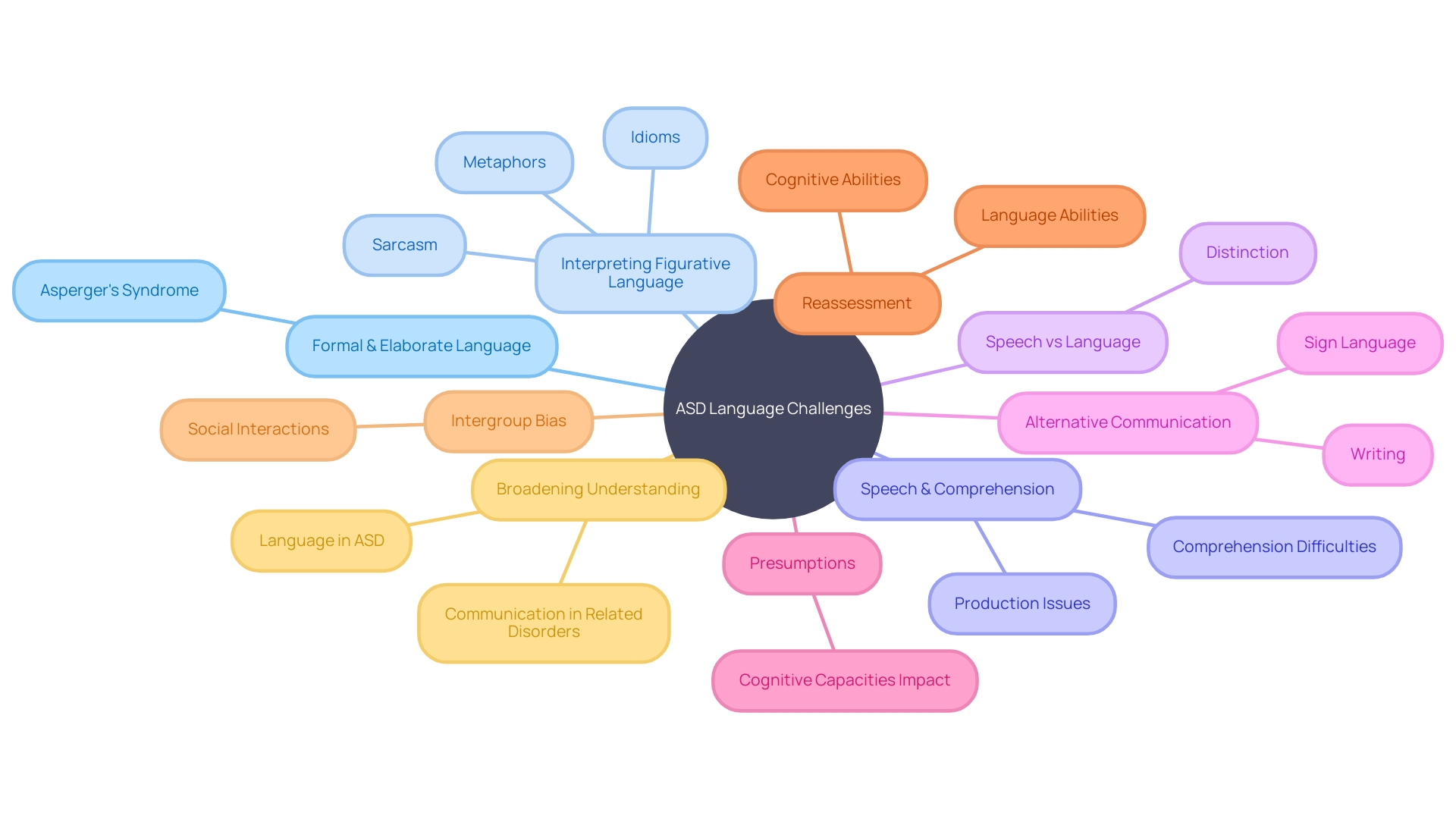
The ability to use language in social situations is a complex skill that involves not just the words we choose, but also how we convey and interpret meaning. For people with , language use tends to be less impaired when compared to those with Autism Spectrum Disorder (ASD). They often exhibit a formal and elaborate use of language; however, interpreting sarcasm, metaphors, and idioms can be challenging for them. In contrast, individuals with ASD may encounter a wider range of language challenges which can involve issues with speech production, comprehension, and the subtleties of social interaction.
Recent studies underscore the importance of distinguishing between speech and language, as they are not one and the same. A person's inability to speak does not necessarily indicate a lack of language capacity. This is shown by people who, despite significant speech limitations, can express themselves through alternative means such as sign language or writing. This difference is crucial because around one-third of people with autism face significant challenges with verbal expression, which can result in presumptions about their cognitive capacities and impede their ability to utilize effective means of interaction.
For example, a profound case that illustrates the disparity between speech and understanding involved a non-speaking autistic teenager who was presumed to be unable to comprehend his surroundings. His behavior was seen as purely disruptive until he communicated 'help me it hurts' using a simple alphabet toy. This incident highlights the critical need for a reassessment of how language and cognitive abilities are evaluated in non-speaking individuals.
Furthermore, investigation into social interaction has unveiled intriguing discoveries about authentic versus feigned smiles and the function of intergroup bias. Studies show that people are inclined to favor those who are more similar to themselves, influencing how we perceive and judge non-verbal cues like smiles. This bias can impact our evaluations of genuineness in social interactions, which are vital to interpersonal connections.
In light of these insights, it is clear that we need to broaden our understanding of language and communication, especially within the context of ASD and related disorders. This knowledge is crucial in developing interventions that respect the individual's unique language capabilities and provide them with opportunities to engage meaningfully in their communities.
In the domain of neurodevelopmental disorders, Autism Spectrum Disorder (ASD) and Autism Spectrum Disorder (ASD) showcase distinct cognitive patterns. Individuals with a certain type of Syndrome usually show average to above-average intelligence. This intelligence is multifaceted, including , which are part of the broader executive functions integral to human cognition. Such functions are foundational to problem-solving, adapting to new situations, and learning from experience. For example, they can have a remarkable ability to retain and manipulate information, a characteristic of strong working memory, which is beneficial for tasks that require holding several pieces of information in mind at once.
On the other hand, Autism Spectrum Disorder encompasses a broader spectrum of cognitive abilities, ranging from challenges with intellectual disabilities to exceptional cognitive skills. The variability in ASD is extensive, reflecting the complex nature of intelligence itself, which is not a single ability but a system of interconnected capabilities. Some individuals with ASD may face difficulties with executive functions such as inhibitory control, which helps with regulating one's actions and behavior, or cognitive flexibility, which is the ability to shift thinking and adapt to changing demands or priorities.
The understanding of these neurodevelopmental conditions is continually evolving with research. Recent studies employing advanced techniques like transport-based morphometry have begun to reveal patterns in brain structure that correlate with genetic variations linked to autism. These insights underscore the importance of considering the full tapestry of cognitive abilities when discussing the Syndrome associated with high-functioning autism and ASD, moving beyond traditional behavioral diagnosis to a more nuanced understanding that may inform personalized approaches to support and intervention.

Asperger's Syndrome (AS) and Autism Spectrum Disorder (ASD) are both part of the same autism spectrum, characterized by a diverse range of behavioral traits and repetitive behaviors. While people with AS might display such as adherence to routines or intense interests as coping mechanisms for anxiety or to attain sensory input, those with ASD often exhibit more overt repetitive actions. These can include physical movements like rocking or hand flapping and a strict observance of routines and rituals.
As per the CDC, ASD is present in up to 1 in 36 people. The American Psychiatric Association's DSM-5 outlines the diagnostic criteria for ASD, including persistent challenges in social communication across multiple contexts, and the display of restricted and repetitive patterns of behavior. These behaviors can manifest as repetitive speech, an overwhelming preference for sameness, and hypersensitivity or lack of sensitivity to sensory information.
It's essential to recognize these behaviors across all ages, as 1 in 45 adults in the U.S. are diagnosed with ASD. Comprehending the distinctions between AS and ASD aids in recognizing the distinct challenges faced by people and customizing support accordingly. Early detection of ASD can have a significant effect on people, providing them with the necessary support and chances to live rewarding lives. Early diagnosis hinges on reliable screening tools, like the Modified Checklist for Autism in Toddlers-Revised (M-CHAT-R/F), though its sensitivity in real-world pediatric settings can be as low as 39%, highlighting the need for more precise screening instruments.
Research into the neurodevelopmental underpinnings of ASD has revealed that brain scans of individuals with autism show variations in brain structure when compared to neurotypical development. While the exact cause of autism remains under investigation, it is widely accepted that it is linked to brain structure or function differences, and not caused by vaccines or parenting styles.
The presence of elevated levels of repetitive behaviors beyond expected developmental periods may suggest a delay in the development of advanced cognitive mechanisms for emotional and behavioral regulation, and it is associated with neurodevelopmental conditions like ASD. This understanding underscores the importance of nuanced approaches to support and intervention for those on the autism spectrum.
Understanding the differences between a specific syndrome and Autism Spectrum Disorder (ASD) is crucial for parents and healthcare professionals alike. Both conditions come under the umbrella of ASD, which is marked by difficulties in social interaction, interaction, and a limited range of interests and behaviors. However, it is crucial to highlight that a certain condition presents with milder symptoms and usually does not involve the language delays commonly seen in classical autism.
Early detection is paramount for both conditions. Studies show that the median age of autism diagnosis is over 4 years old, with even greater delays among children from minority backgrounds. These findings highlight the necessity for more robust and equitable screening tools. The Modified Checklist for Autism in Toddlers-Revised with Follow-Up (M-CHAT-R/F), while useful, has demonstrated variable accuracy in different settings, particularly for girls and children of color.
Interventions tailored to the unique needs of each child can significantly enhance their developmental trajectory. Whether it's through Individualized Education Programs (IEPs) in schools, specialized instruction, or sensory integration therapy, personalized support can make a substantial difference. Although there are no medications specifically for high functioning autism, certain treatments can alleviate co-occurring conditions, thereby improving quality of life.
Globally, approximately 1 in 160 children are diagnosed with ASD, according to the Centers for Disease Control. With , coupled with personalized interventions, there is a great potential to improve social skills, language abilities, and adaptive behaviors, thus assisting these children in leading more satisfying lives.
Therapeutic strategies for individuals diagnosed with , including those previously diagnosed under the term Asperger's Syndrome, are personalized and multifaceted. This tailored approach is crucial because each person on the spectrum has a unique set of abilities and challenges. As such, treatment plans often incorporate behavioral interventions, speech and language therapy to aid communication, occupational therapy to improve daily functioning, and social skills training to enhance interaction with others. The emphasis on early and accurate diagnosis is underscored by organizations like The Autism Community in Action (TACA) and the developments from NeuroQure, which underscore the potential for improved outcomes with timely interventions. With the understanding that the nomenclature of conditions like ASD is evolving, with a move away from eponymous labels to more descriptive terms, it remains pivotal to focus on effective, evidence-based treatments that are adaptable to the diverse needs within the autism community.
In conclusion, understanding the distinctions between Asperger's Syndrome and Autism Spectrum Disorder (ASD) is crucial for parents and healthcare professionals. Both conditions fall under the umbrella of ASD, which encompasses a range of challenges in social interaction, communication, and behavior. Early and accurate diagnosis is vital, as it allows for personalized interventions and support.
Treatment approaches for ASD are multifaceted, incorporating behavioral interventions, therapy, and social skills training. By gaining insights into these aspects, parents and healthcare professionals can empower themselves with expert advice to better support individuals with ASD and help them lead fulfilling lives.
Empower yourself with expert advice and better support individuals with ASD!
What is Asperger's Syndrome?
Asperger's Syndrome was once considered a distinct disorder within the Autism Spectrum Disorder (ASD) category. It is characterized by specific social and communicative challenges while maintaining strong language abilities and normal intellectual development.
Why has the classification of Asperger's Syndrome changed?
In 2013, Asperger's Syndrome was integrated into the broader diagnosis of Autism Spectrum Disorder (ASD) in the DSM-5. This shift reflects a more inclusive understanding of autism, acknowledging the diverse spectrum of symptoms and behaviors.
What are the key differences between Asperger's Syndrome and Autism Spectrum Disorder?
While both fall under ASD, individuals with Asperger's Syndrome typically exhibit milder symptoms, strong language skills, and normal intellectual capabilities. In contrast, ASD can include a wider range of challenges, including significant language delays and intellectual disabilities.
How does social interaction differ between Asperger's Syndrome and ASD?
People with Asperger's may struggle with non-verbal cues and sustaining relationships, while those with ASD might face more severe challenges in initiating and maintaining social exchanges, including a lack of interest in social activities.
What cognitive and behavioral patterns are associated with Asperger's Syndrome and ASD?
Individuals with Asperger's often have intense interests and prefer routines. ASD encompasses a broader range of cognitive abilities, from intellectual disabilities to exceptional skills, reflecting a more heterogeneous condition.
How do language skills vary between individuals with Asperger's and those with ASD?
Individuals with Asperger's typically have less impaired language use and may struggle with figurative language, while those with ASD may experience a wider range of challenges, including issues with speech production and comprehension.
What are the common behavioral characteristics of Asperger's Syndrome and ASD?
Both conditions can exhibit repetitive behaviors; however, individuals with Asperger's may show these as routines or intense interests, while those with ASD may display more overt repetitive actions like rocking or hand-flapping.
Why is early diagnosis important for Asperger's and ASD?
Early detection is crucial for providing timely interventions, which can significantly improve developmental trajectories. Studies indicate that median diagnosis ages are often too late, emphasizing the need for effective screening tools.
What treatment approaches are available for individuals with Asperger's and ASD?
Treatment is personalized and may include behavioral interventions, speech and language therapy, occupational therapy, and social skills training. Early and accurate diagnosis is essential for improving outcomes.
What are the societal implications of understanding these conditions?
Recognizing the nuances between Asperger's Syndrome and ASD promotes a more inclusive and empathetic environment, helping society better understand and support individuals on the autism spectrum.